Today’s post will be a little bit different, shorter, and to the point, given the importance of the information shared, especially the first one. After the “sodium” debacle, meaning how a few corrupt doctors and researchers misguided the entire world into believing “salt=bad”, the second biggest debacle was and still is animal protein = bad for you. I do not possess the willpower, the time or the willingness to debunk every paper that pushes “meat is bad for you”, there are dozens of big social media accounts dedicated to this, but one specific lie I would like to bring to light.
Protein intake and risk of urolithiasis and kidney diseases: an umbrella review of systematic reviews for the evidence-based guideline of the German Nutrition Society
Methods
PubMed, Embase and Cochrane Database of SRs published until 12/2022 were searched for the respective SRs with and without meta-analyses (MA) of randomised controlled trials or cohort studies. For assessments of methodological quality and of outcome-specific certainty of evidence, a modified version of AMSTAR 2 and the NutriGrade scoring tool were used, respectively. The overall certainty of evidence was assessed according to predefined criteria.
Results
Six SRs with MA and three SRs without MA on various kidney-related outcomes were identified. Outcomes were chronic kidney disease, kidney stones and kidney function-related parameters: albuminuria, glomerular filtration rate, serum urea, urinary pH and urinary calcium excretion. Overall certainty of evidence was graded as ‘possible’ for stone risk not to be associated with HPI and albuminuria not to be elevated through HPI (above recommendations (> 0.8 g/kg body weight/day)) and graded as ‘probable’ or ‘possible’ for most other kidney function-related parameters to be physiologically increased with HPI.
Conclusion
Changes of the assessed outcomes may have reflected mostly physiological (regulatory), but not pathometabolic responses to higher protein loads. For none of the outcomes, evidence was found that HPI does specifically trigger kidney stones or diseases. However, for potential recommendations long-term data, also over decades, are required.
The conclusion speaks for itself, there is little to no evidence that high protein intake causes, or induces different types of kidney diseases, or that high protein does so via damaging metabolic pathways, rather the changes come from the body attempting to “fix” something else.
A large proportion of studies covering high-protein with kidney “dys” function often ignore the most common, vastly more damaging, common denominator. Carbohydrate-rich diets may increase the risk of CKD development in non-DM subjects. Another recent article:
Associations of low-carbohydrate with mortality in chronic kidney disease
Results
Most macronutrients were non-linearly associated with all-cause mortality risk, including carbohydrates and sugar. Participants with CKD had lower mortality risk when consuming 30–45% energy from carbohydrates (average HR 0.76, 95%CI 0.62–0.93, compared with 60%), 5–20% energy from sugar (average HR 0.75, 95% CI 0.59–0.96 compared with 40%). Replacing the energy intake from carbohydrates with protein (up to 30%) and/or replacing the sugar with non-sugar carbohydrates (up to 55%) reduced the all-cause mortality risk, while the total energy intake remained constant.
People with Chronic Kidney Disease (CKD) who substituted their energy source from mainly carbohydrates and sugar to protein, and we are not talking about a drastic shift such as full-carnivore, had better long-term outcomes and reduced all-cause mortality risk, meaning lower risk of any other type of disease, infection, etc. In line with the first paper.
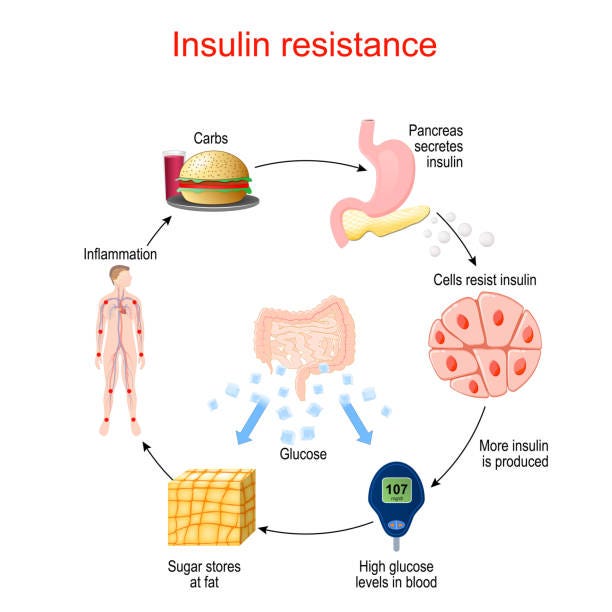
A Korean study using 10,000 participants found that a Low-fat/High high-carbohydrate intake was associated with an increased risk of developing CKD. This was independent of protein intake. Besides a myriad of different pathogens (bacterial, fungal/yeast), chronic infection (such as EBV, CMV, HIV…see a trend ? No ? Just me ?), the two most common, and “first contributors” to the development and aforementioned pathogenic causes for kidney disease are hyperinsulinemia (excess insulin in the blood) and Insulin Resistance.
Insulin Resistance (IR) as the name implies is the progressive resistance of your cells towards the hormone insulin, which is often the “first stage” in this cascade, hyperinsulinemia is a compensatory response to IR, but at a point in time, since your cells don’t respond to insulin as effective as under normal metabolic condition, insulin will be left to be degrade in the kidney.
Consuming carbohydrates, even “in occasional excess” is not exactly the problem, the problem lies in the principles of thermodynamics and energy balance. An extremely simplified version of these mechanisms.

These complex interactions between carbohydrates, glucose, and its interactions with other proteins, lipids, and cell responses will contribute significantly to the development of the disease itself. Adding salt to injury (or in this case, ironically, sometimes these complex interactions remove the salt from you =P) will create bioenergetic feedback loops that will decrease how efficiently your cells create, use, and store energy, thus creating a self-perpetuating loop.
If you have been reading this Substack for a while or health-related content, odds are you are very aware of how amino acids play an important role in both health and disease, and supplementing certain amino acids can improve symptoms or outright help you recover. Tryptophan is the primary and most pertinent one, followed by N Acetyl Cysteine. Now, could lower or higher protein impact immunological function ?
Protein Energy Malnutrition Impairs Homeostatic Proliferation of Memory CD8 T cells
Nutrition is a critical but poorly understood determinant of immunity. There is abundant epidemiological evidence linking protein malnutrition to impaired vaccine efficacy and increased susceptibility to infections; yet, the role of dietary protein in immune memory homeostasis remains poorly understood. Here we show that protein energy malnutrition (PEM) induced in mice by low-protein (LP) feeding has a detrimental impact on CD8 memory. Relative to adequate-protein (AP) fed controls, LP feeding in lymphocytic choriomeningitis virus (LCMV) immune mice resulted in a 2-fold decrease in LCMV-specific CD8 memory T cells. Adoptive transfer of memory cells, labeled with a division tracking dye, from AP mice into naive LP or AP mice demonstrated that PEM caused profound defects in homeostatic proliferation. Remarkably, this defect occurred despite the lymphopenic environment in LP hosts. While antigen-specific memory cells in LP and AP hosts were phenotypically similar, memory cells in LP hosts were markedly less-responsive to poly(I:C)-induced acute proliferative signals. Furthermore, upon recall, memory cells in LP hosts displayed reduced proliferation and protection from challenge with LCMV-clone 13 resulting in impaired viral clearance in the liver. The findings show a metabolic requirement of dietary protein in sustaining functional CD8 memory and suggest that interventions to optimize dietary protein intake may improve vaccine efficacy in malnourished individuals.
I would personally ignore that last phrase…
Insufficient protein intake directly affects the function and proliferation of CD8+ memory cells, the “fast responders” of infections, given they are the first to “appear” within 24 hours of a pathogen activating your immune system. While the cells from “normal” and “low” protein were similar, the memory cells from the inadequate protein group were less responsive, anergic, and less proliferative (meaning it is unable to produce more copies of itself) thus leading to impaired capacity to clean infections. In case you need a refresher, from here.
Strong SARS-CoV-2 N-specific CD8+ T immunity induced by engineered extracellular vesicles associates with protection from lethal infection in mice
Broad and strong memory CD4+ and CD8+ T cells induced by SARS-CoV-2 in UK convalescent individuals following COVID-19
In mild cases, higher proportions of SARS-CoV-2-specific CD8+ T cells were observed.
Impaired Cytotoxic CD8 + T Cell Response in Elderly COVID-19 Patients
SARS-CoV-2 infection induced a vigorous cytotoxic CD8+ T cell response. However, this cytotoxic profile of T cells was not detected in COVID-19 patients over the age of 80 years. Thus, the absence of a cytotoxic response in elderly patients might be a possible reason for the more frequent severity of COVID-19 in this age group than in younger patients.
In regards to kidney disease, but easily extrapolated to many other conditions, improper protein intake leads to improper immune function which will definitely contribute to the progression of many chronic conditions by failure to maintain proper immunological responses. So one could argue failure to meet adequate protein intake is one of the main causes for acquiring different types of immune dysfunction (I rather not use the term deficiency, since when you introduce adequate, good quality protein, most tend to recover).
The most complex aspect of diet and our immune system is slowly being unveiled, and that aspect is the microbiome. Any change, either via antibiotics, infections, or inflammation can affect the microbiome, diet especially can affect it short and long-term.
The influences of low protein diet on the intestinal microbiota of mice.
Given that the goal here is to be more informative rather than breaking down complex metabolic and immunological pathways I will leave some observations that came after almost 20 years of learning.
One of the primary distinctions when consuming more protein, is protein quality, and I don’t mean privileged “grass-fed” marketing, but cuts
Different animals have different amino acid composition, but different cuts have different nutritional values
For older people, people with chronic disease, and especially people with gut dysbiosis, and gut inflammation, you need “easily digestible” sources of protein
Softer cuts, minced/shredded meat are easier for the gut to digest and absorb
The best and easiest protein to absorb and get all the benefits of is whey protein, followed by eggs
The liver is the most nutritious protein source in nature… if you can tolerate the taste
The older or sicker you are, the more protein you need, and you need easier to digest and absorb protein. Since CD8 cells are so important, I wonder (paper below here)…
The paywalled version, titled Vaccine-induced CD8+ T cells are key to protection from SARS-CoV-2.
Using molecular signatures from vaccinated samples, we annotated antigen-specific CD8+ T cells in additional published datasets13, including samples from patients with COVID-19 (refs. 44,46). In these samples, we also leveraged immune repertoire information to link antigen-specific CD8+ T memory precursor cells with their differentiated progeny. We found that disease severity and outcome correlated not only with the abundance of the CD8+ T memory precursor cells but also with the molecular state of their descendants, and in particular, we found that donors who manifested extensive TCR sharing between memory CD8+ T precursor cells and cytotoxic CD8+ T cell progeny were associated with a milder clinical course. These results exemplify a potential mechanism by which cellular immunity may play an important role in resolving viral infection.
(This has been my argument since late-2020…)
Bacterial strains modulate CD8+ T cell function and cancer immunity
I sure hope vaccines don’t affect the microbiome (this is called foreshadowing).





It didn't exactly fit in the article itself, but this paper is rather significant. -> Maltodextrin Consumption Impairs the Intestinal Mucus Barrier and Accelerates Colitis Through Direct Actions on the Epithelium
"These results suggest MDX disrupts the balance of epithelial cell differentiation and proliferation to contribute to disease pathogenesis through direct and indirect actions on the intestinal epithelial barrier."
https://www.frontiersin.org/articles/10.3389/fimmu.2022.841188/full
I have stage 3a kidney failure. My GFR ranges from 60 to 45 on some days. It doesn't seem to matter how much fluid I drink because I always try to stay hydrated but it fluxuates often. I have come up with a standard for myself in which I figured I would drink 1/2 my body weight of fluids in ounces meaning, if I weigh 140lbs I drink 70 to 75oz of water, kombucha, tea, raw milk & juices during the day. Do you think this is sufficient amount of fluids? too much or too little? I eat organic, homegrown foods with very little purchased from the Monsanto grocery stores.
I went the local University and saw a nephrologist a year or two ago and she told me that there was nothing she could do for me to increase my kidney numbers until I get worse and then she suggested dialysis. Sick care is NOT health care. These people are educated idiots.