Accelerated vascular ageing after SARS-CoV-2 infection
There is more to it than meet the eyes
This is an impromptu article, I will refer to a few pertinent, longer, more complex, and comprehensive articles. As much as I enjoy breaking down complexity in different topics, with a strong focus on SARS-CoV-2, I often also want to back any old or new assertion or hypothesis with data, or simply bring awareness to important information or data.
One long-standing topic in my publication has been the drastic and often lasting impact SARS-CoV-2 has on our circulatory system, both the normal one that everyone has some awareness of, and the capillary, the microcirculatory system, which gets little attention but has the most significant and long-term impact on human health. Pertinent articles below.
Accelerated vascular ageing after COVID-19 infection: the CARTESIAN study
In case my readers are asking themselves what CARTESIAN means, it is an acronym for “Covid-19 effects on ARTErial Stiffness and vascular AgeiNg”, it is a large-scale, international (38 centers in 18 countries) study that aims to observe the vascular impact of a Covid infection. I will already preface this, the study was done between 2020 and 2022, and just 10% of the patients were vaccinated.
Although I do want to bring something to your attention, something I picked up in the first Pfizer and Moderna trial, and brought up on social media. In the Supplementary Data Table 13, you can clearly observe a trend that remained true for 18 months since the first mass vaccination effort, this trend changes and were skewed completely towards every side when reinfections became common place, followed by secondary infections.
Vaccinated people experienced either mild infection or otherwise experienced a disproportionate number of severe infections, 15% each, with very low numbers of moderately infected. A lot more goes to it, but I digress.
There are a few ways to measure your vascular age, and one of those is Pulse Wave Velocity. This test measures the speed at which fluid travels through the arteries, the slower, the younger your vascular system theoretically is, the older, faster, indicating your arteries are calcified and stiff. If you are interest in how the test is done, it is quite simple, a sensor in the carotid artery, another in the femoral, and the system measures the delay it takes for the wave to travel between both.
It is now accepted that estimating the PMV has a strong predictive power on the incidence of future cardiovascular events and cardiovascular disease, each 1 m/s increase is associated with an increase of all-cause and cardiovascular mortality by a significant margin. In different age groups too.
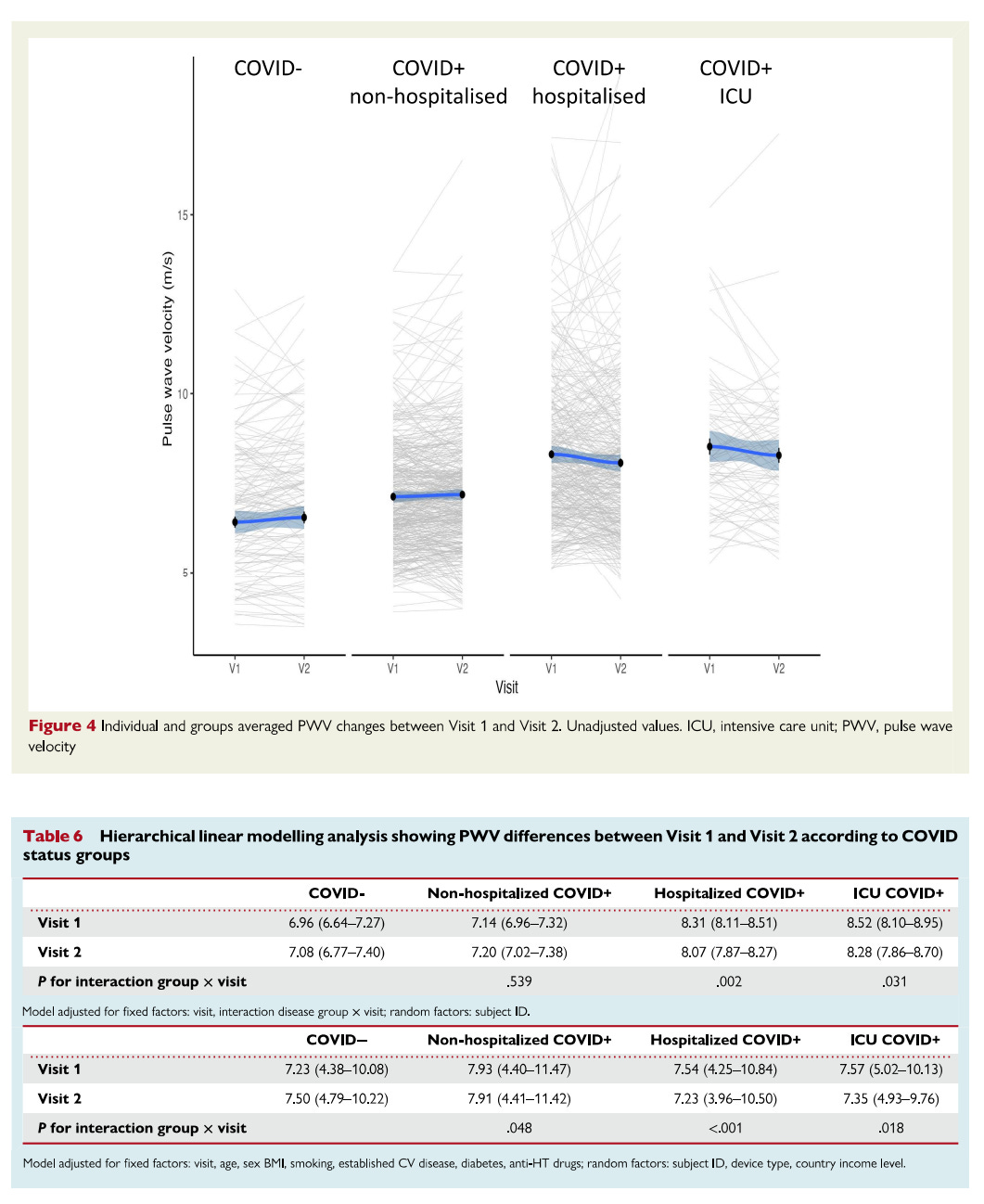
The 2,390 participants in this study were divided into 4 groups, Covid-negative, which acted as controls, Covid+ Non-hospitalized, Covid+ Hospitalized, and Covid+ Hospitalized ICU, which were tested at an average of 6 months post-infection (some 3, other 9 months post-infection), and the follow-up was an average 9 months (some at 9 others 15 months) post-infection to assess the long-term effects.
The authors did a good statistical analysis, adjusting for all confounding variables (age, sex, BMI, blood pressure, people who had cardiovascular disease already, smoking, and other factors). Compared to Covid Negative patients, any person who had a Covid infection had a significant increase in their PWV, and similar to so many other studies, the higher the infection severity, the more impact your body experiences.
Non-hospitalized COVID+: +0.36 m/s higher.
Hospitalized COVID+: +0.37 m/s higher.
ICU COVID+: +0.79 m/s higher.
An increase of +0.5 m/s corresponds to approximately 5 years of accelerated vascular aging and a 3% increased risk of cardiovascular events. For the ICU patients, the increase of nearly +0.8 m/s is a very significant marker of vascular damage. I would strongly pay attention to the non-hospitalized Covid+ group, because experiencing roughly 3 years of vascular aging per mild infection isn’t exactly a pathway to long-term health. That is the average, a breakdown between men and women gives you a distinct perspective.
In women, non-hospitalized patients had their PWV increased +0.55 m/s compared to controls. hospitalized +0.60 m/s and ICU patients +1.09, experiencing significant vascular damage. In men, there is no statistical significance between any severity of infection. The second visit, the follow-up to assess the long-term impact of the infection, gives us a better and more positive picture.
Although the initial impact demonstrates accelerated vascular aging, with women bearing the brunt of it in this study, the follow-up visit gives us a more positive outlook. This accelerated aging of the vascular system is not permanent, there is evidence (image above) that over a year post-infection, repair of the vascular system occurs, although a return to baseline doesn’t occur.
The Covid negative group experiencing an increase in their values is understood as normal vascular aging. SARS-CoV-2 infection and its following inflammatory response trigger pro-atherogenic responses, in simple English, the clogging of your arteries. This was recently observed in China, where coronary artery lesions were evaluated (and here the majority of patients were male, but also older).
It is a different approach, and the patients already had some sort of coronary disease, but there is significant evidence of both the onset of new, and especially the acceleration of subclinical and clinical pathology. Even recently I have written on the effects of the virus on the vascular system.
The primary form of damage is via endothelial dysfunction, by directly using ACE2, the virus can directly infect the cells in the vasculature, leading to progressive inflammation and damage, which in turn creates a feedback loop. Viral fragments can persist in the endothelial cells long after the virus is dead, and create a persistent inflammatory environment.
Systemic inflammatory responses, as we saw recently, will also cause a significant burden throughout the whole body, and this will directly and indirectly burden the vascular system. Another way is simply the distinct immunological responses between both sexes, as women often present with a much stronger and faster immune response to anything, it is why they are more predisposed to prolonged inflammatory diseases and autoimmunity. Given the virus causes a hormonal havoc and can manipulate Estrogen Receptors, it could, in theory, cause such accelerated aging too.
But my publication wouldn’t be called Things Hidden in Complexity if there wasn’t more to it. Although the mechanisms for this paper are a multitude, there is one specific mechanism that in the long term may cause the greatest increase in cardiovascular burden. One, I have brought up not only multiple times but since 2020.
Cardiorenal outcomes after herpes zoster reactivation in COVID-19 survivors from a global TriNetX study
Herpes zoster (HZ) has emerged as a post-viral complication in COVID-19 survivors, but its long-term clinical impact remains uncertain. This retrospective cohort study utilized the TriNetX Global Collaborative Network to evaluate whether HZ reactivation after COVID-19 is associated with increased risks of mortality, cardiovascular, and renal outcomes. Adults diagnosed with HZ within one year of COVID-19 were propensity score–matched 1:1 with controls without HZ. A total of 48,442 matched patients were followed for three years. Compared with controls, HZ patients had significantly higher risks of major adverse cardiovascular events (HR: 1.38, 95% CI: 1.30–1.46), acute kidney injury (HR: 1.67, 95% CI: 1.55–1.80), and renal function decline defined by eGFR < 60 mL/min/1.73 m² (HR: 1.28, 95% CI: 1.20–1.37). Although no significant difference in overall all-cause mortality was observed across the full follow-up period, time-stratified analysis revealed a biphasic pattern: patients with HZ had lower mortality risk during the first 90 days but showed significantly higher mortality from day 91 to three years post-COVID-19 (HR: 1.33, 95% CI: 1.24–1.44). Subgroup analyses consistently identified older age, chronic comorbidities, impaired renal function, and systemic inflammation as risk enhancers across outcomes. These findings suggest that HZ reactivation after COVID-19 signals a vulnerable subgroup predisposed to cardiorenal complications. Targeted follow-up and risk-based interventions are warranted in this population.
Throughout 2021, I brought up, persistently, how most analyses in regards to anything related to SARS-CoV-2 were missing timing windows, most analyses were centered around the first 2, 4, or even 12 weeks post-infection, or post-exposure (mRNA vaccine). And that window would skew any honest interpretation of real-world data.
No all-cause mortality differences were observed during the first 90 days, but at day 91 up to three years post-Covid infection, there was a significant increase. Among these patients, older age, chronic comorbidities, impaired renal function, and systemic inflammation increased the risk of these outcomes.
A 38% increase in the risk of suffering a heart attack, stroke, or worse, cardiovascular-related death. Acute kidney injury showed an even larger increase, 67% of developing AKI, and a 28% higher risk of developing chronic kidney disease over time, indicating a serious increase in microvascular damage. Herpes Zoster itself increases the risk for vascular disease in the long term. A somewhat comprehensive breakdown of latent viruses and infections below.
Latent viruses contribute to many diseases over the long term, which is easy to miss, given that subclinical damage is not the focus of healthcare, nor does any healthcare system tackle such an endeavor at a societal level. On the bright side, data over the long term indicates that there is always recovery, or that damage is reversible, even though you slightly lose a bit of your baseline, which arguably you could recover over time with exercise.
That is why I insist on repeating myself throughout this year on limiting inflammation and supplementing with your choice of supplements, in this particular case, the old combo works wonder, that being Taurine + Vitamin C, Quercetin, Olive Leaf Extract (20% Oleuropein) being of great aid to it, Vitamin D which will help the immune system recover and keep Herpes at bay. Pushe comes to shove, BPC-157 + TB 500 to achieve fast, significant, systemic recovery, and supplementation to the finish line.
Also, a reminder.
If you are a paid subscriber, thank you for supporting my work. If you are not, consider becoming one at any time.











The focus here was covering the trends and effects, rather than a precise breakdown of the molecular and immunological pathways (which are around my Substack, some linked here).
I will keep repeating myself on the necessity of supplementation, at least a few things, because over time, these things will stack.
My next article will be either simpler and shorter, or a sequel to my Language - The Genocidal Organ article.
Because we now live in a post-Genocidal Organ world. Go watch the animated movie if you haven't.
Speaking of Shingles
https://geoffpain.substack.com/p/shingrix-disaster-due-to-endotoxin