The brain's housekeeping - Glymphatic System
Part I
There is a announcement and some important information pinned in the comment section of this article.
This piece is a direct continuation of my Misfolded Proteins article.
Protein folding or failure to (misfolding) is one of the holy grails of biology, you solve that, you solve a good portion of the puzzle that is life, as previously mentioned. So I will write a somewhat friendly article on how the body deals with bad proteins. First, we need a short description of the cells in our nervous system and brain.
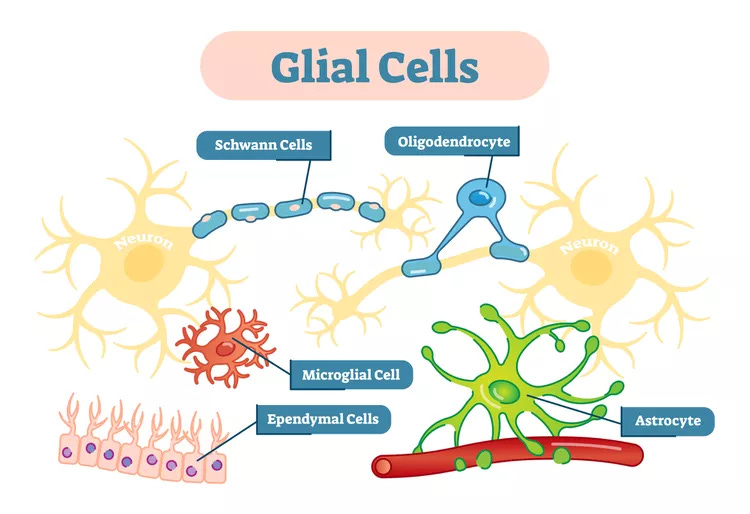
What are glial cells ?
Glial cells are the cells that support the neurons (nerve cells) in your brain, they are the supporters of your brain health =D.
There are five types of glial cells:
Astrocytes
Oligodendrocytes
Microglia
Ependymal cells
Radial glia
Astrocytes (also named astroglia) are the most common type of glial cell, and they play multiple roles in the brain such as forming the Blood-Brain Barrier, which is basically the brain filtering system to keep anything that isn’t supposed to be there, out. The BBB can be described as your brain's first line of defense, in and on itself it can filter “misfolded” proteins, and the BBB itself is protected by a barrier the “Glial barrier. You can imagine the glial barrier as the image above, an astrocyte using the end of its tentacles to wrap around “stuff”.
The “tight” junctions formed by this glial barrier are not tight enough to stop tau, and amyloid beta from passing through, but the tight endothelial junctions at the BBB prevent. Failure (permeability) in the BBB = neurological inflammation, progressive neurodegeneration.
They also regulate neurotransmitters and recycle them after they are done, they also clean up the cell waste after that. Another two important functions are regulating the activity of axons (the long part of neurons and nerves cells that transmits messages between them), and regulating brain energy metabolism.
Oligodendrocytes are responsible for producing myelin, a fatty substance that insulates the axons of neurons, allowing for the rapid transmission of electrical impulses and playing a crucial role in the functioning of the nervous system.
And we have microglia, the immune cells of the nervous system, they are responsible for responding to infections, phagocytosis (engulfing and digesting cellular debris, pathogens, and damaged neurons), and regulating immune reactions, inflammation, and tissue repair. They are also responsible for synaptic pruning, and removing excess synapses.
What is the glymphatic system ?
If you never heard of the glymphatic system, it wouldn’t be surprising. While its proposition is old, evidence was only properly discovered in 2012/2013. I will now refer to it as GS. The name comes from combining glial and lymphatic, given the involvement of glial cells in the GS and its similarity with the lymphatic system. The shortest way to understand the GS is to understand the lymphatic system.
The lymphatic system (LS) is similar to the vascular system, but with very distinct functions, it is main goal is maintaining fluid balance, filtering and disposing of harmful substances, and especially importantly supporting the immune system. Lymph is the clear liquid that surrounds cells (science name - interstitial fluid), and the lymph nodes are the filters, they can trap, and remove any foreign substance, such as bacteria, viruses, cancer cells, excess fluid from inflammation, any foreign particles that enter your body through the respiratory or digestive system.
The GS is very similar to the LS, but as the name implies it acts solely on the nervous system and the brain. The glymphatic system functions primarily during sleep, and its main purpose is to clear waste products from the brain. While we sleep, glial cells, particularly astrocytes, become more active. These cells help to regulate the flow of cerebrospinal fluid (CSF) through the brain tissue. The CSF washes through the brain, carrying away waste products, such as amyloid beta and tau proteins, which are associated with conditions like Alzheimer's disease.
The glymphatic system's role in waste clearance is crucial for maintaining brain health. Impairments in this system have been linked to neurodegenerative diseases. And one of the ways your glymphatic system and cells execute these critical functions is by Aquaporin-4, a protein expressed in astrocytes, and crucial to enable the movement of fluids in the brain, it is abundant in the Aquaporins. Dysfunction of AQP4 is directly correlated with neurodegeneration.

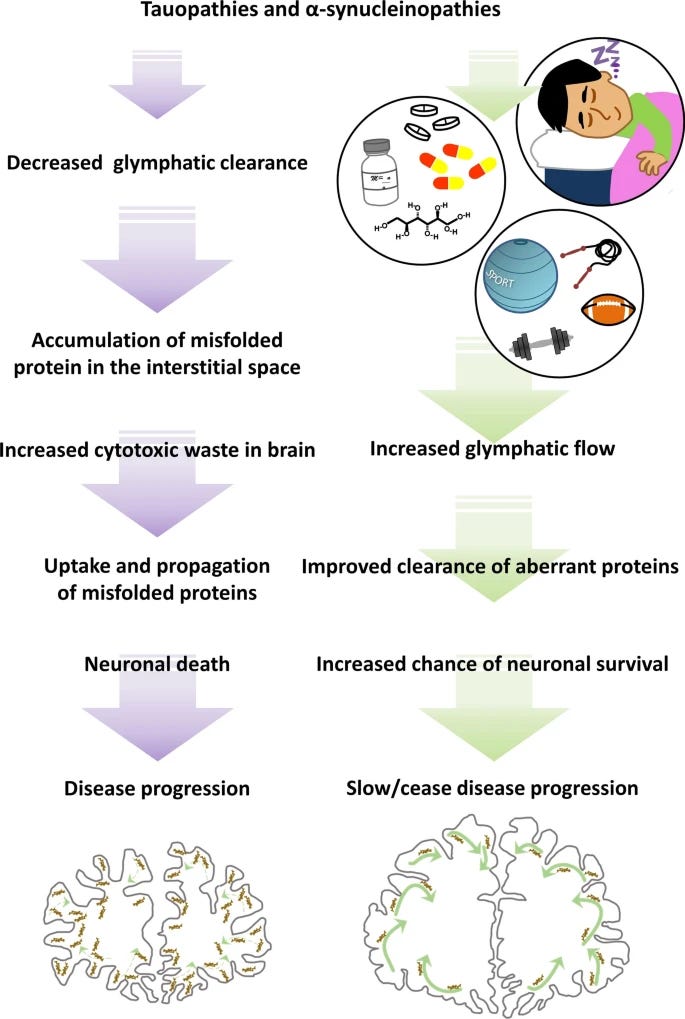
If you recall, protein shape dictates function, so there are three “states” a protein can have in your body. Soluble, meaning it has proper shape but it can travel in the body and it has many functions, a normal protein, and a “insoluble” protein, a misfolded protein. Soluble proteins, and “normal” proteins can both be dissolved by water and other enzymes (lipases, proteases, and many other -ases) while misfolded proteins, and “aggregates” are resistant towards them.
Your cells can still break down misfolded proteins at a certain threshold, if they aggregate and become “too big”, accumulation ensues. Each “misfolded” protein has a distinct mechanism, both physiological and pathological, such as tau and α-synuclein but recent evidence points towards the same “initiator event”, it is not the misfolding itself after all your body has almost a dozen ways to deal with that event, or even the aggregation itself, but clearance.
If clearance is disrupted, impeded, or otherwise fails, it can be the event that leads to pathology. The following from here.
Accumulation of neurotoxic forms of amyloid-β (Aβ) and tau proteins is the pathological hallmark of Alzheimer disease (AD)
Excess deposition of Aβ results from an imbalance between its production and clearance; in both early-onset and late-onset forms of AD, Aβ clearance seems already impaired at the prodromal stage
Aβ is removed from the brain by various overlapping and interacting clearance systems: degradation, blood–brain barrier (BBB) transport, interstitial fluid (ISF) bulk flow, and cerebrospinal fluid (CSF) absorption into the circulatory and peripheral lymphatic systems
An unanswered question so far is if correction of the glymphatic system and other mechanisms is achieved by pharmacological or natural supplementation, can the body deal with the “big aggregates” that induce disease ?
The most recent evidence demonstrates that the body can synergize using both the central (nervous system) and peripheral (outside the nervous system) clearing systems by using a novel approach to delivering a mimic of amyloid beta antibodies to the brain, reducing the amyloid burden inside the brain by 97%, and outside by 73%.
In another recent study, a nanoformulation (for easier and more efficient delivery to the brain) of Alpha Mangostin, a polyphenol, a powerful antioxidant derived from Garcinia mangostana, demonstrated that it could fix dysfunctional microglia and impressively relieve the symptoms and neurological changes in neurodegenerative diseases. It achieves this by metabolic reprogramming them. Quercetin, Fisetin, Curcumin are cited in the paper.
Other methods from The Sleeping Brain: Harnessing the Power of the Glymphatic System through Lifestyle Choices.
Omega-3 Consumption: They also exhibit anti-amyloidogenic activity, modulate aggregation and decrease downstream toxicity [19]. Dietary intake of n3-PUFAs improved cognitive decline in mild Alzheimer’s disease [19]. Supplementation demonstrates higher CSF influx and clearance, with AQP4 remaining polarized at the astrocytic endfeet, increasing the speed of glymphatic clearance [19].
Intermittent Fasting: Intermittent fasting ultimately downregulates the expression of AQP4-M1, decreasing the AQP4-M1/AQP4-M23 ratio, and therefore increases AQP4 polarization along the paravenous space, boosting glymphatic clearance
Sleeping Position: Glymphatic transport is most efficient in the right lateral sleeping position, with more CSF clearance occurring compared to supine and prone
Our favorite usual suspects also positively influence the glymphatic system. Metformin and Berberine. This second paper is titled Natural products and brain energy metabolism: Astrocytes in neurodegenerative diseases, with many other proposed natural supplements.
From my perspective, yes, we can deal with even the “big aggregates”, even with natural supplements, but a lot of work must be done (it will be accelerated by generative models, AI, and deep learning =) ).
Inflammation and its effects on the brain housekeeping system
While neurodegeneration has many causes, such as TBI (direct injury to the brain), viral or bacterial neurotropism (the pathogen getting inside the brain), autoimmune reactions, a proposed mechanism in the onset of neuroinflammation is the impairment of the lymphatic system, aggravating the inflammatory process by depressing the clearances of inflammatory proteins from the brain.
Changes in the AQP4 will inevitably lead to changes in how the body deals with inflammatory proteins and “waste”, but as with most neurological-related things, it has a dual role. Under specific circumstances, some of the changes in AQP4, directly affecting the glymphatic flow can result in a lesser inflammatory response. Short-term gains, long-term pains, because this will create lasting low-grade inflammation which accelerates neurodegeneration.
All of this is occurring inside the brain, so can the outside of the brain, such as systemic inflammation lead to neuroinflammation ? Our old friend Endotoxin (LPS) is heavily implicated in neurodegeneration, and its systemic presence is enough to induce the expression of inflammatory proteins in the brain, such as TNF Alpha, IL-1Beta, and NF-kB p65.
The systemic response towards inflammatory insult will inevitably lead to pro-inflammatory proteins (cytokines) to sometimes activating the capillaries which in turn can induce the secretion of other cytokines in the perivascular space. Depending on the “size” (molecular weight), they can also cross a healthy BBB. A compromised BBB will inevitably lead to not only unwanted inflammatory proteins getting in but also foreign substances, which will create a vicious cycle of inflammation and progress neurodegeneration.
Many patients with neurological diseases, such as Alzheimer's, Parkinson’s, and Huntington’s all have dysfunctional Blood-Brain Barriers. When your brain gets rid of waste, your liver is responsible for cleaning it out, so liver dysfunction adds insult to injury.
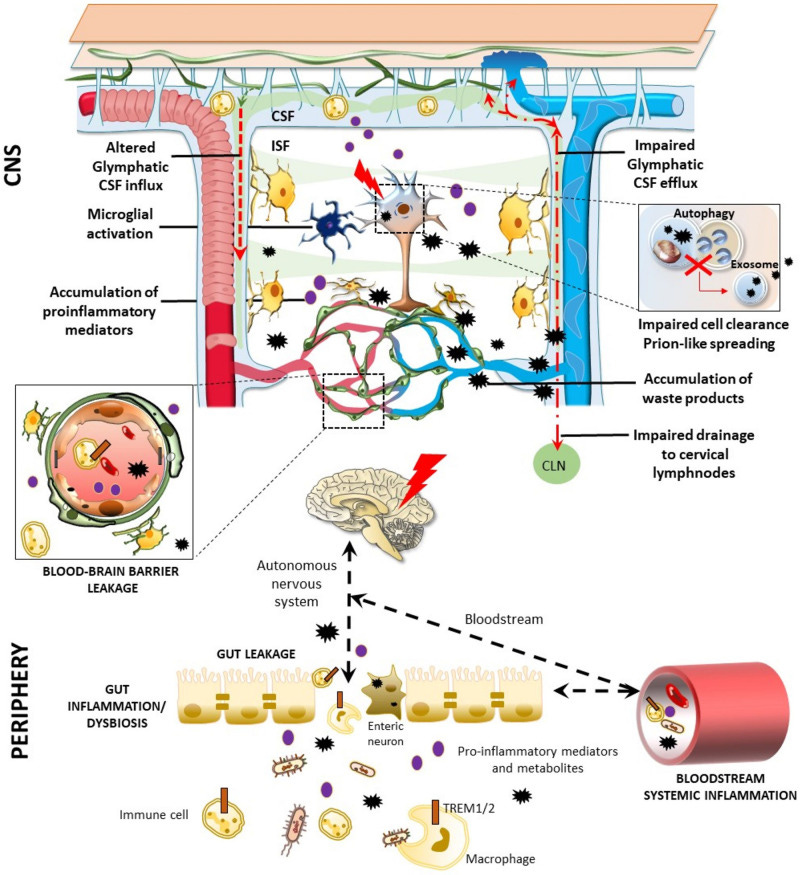
“Propagation of tau and α-synuclein in the brain: therapeutic potential of the glymphatic system” is a fairly extensive paper with detailed information. The following quotes if you are short on time or attention, or for some other reason.
In the context of tauopathy, we recently examined the relationship between glymphatic inflow and clearance of tau from the cortex of a transgenic mouse model of frontotemporal dementia [50]. We demonstrated that in the transgenic mouse brain, glymphatic function was impaired and the level of AQP4 polarisation to astrocytic endfeet was similarly reduced. We also showed that the degree of cortical tau deposition negatively corresponded to the level of glymphatic function in the healthy mouse cortex, alluding to the inverse relationship between the extent of glymphatic function and the degree of tau deposition in the rodent brain. We went on to show that pharmacological blockage of AQP4 resulted in the disruptions of glymphatic inflow and clearance of tau from the brain [50], strengthening the link between AQP4, glymphatic function and tau clearance. Together, these data give strong evidence to suggest that reducing the glymphatic clearance of tau may potentiate the neurodegenerative disease process, perhaps by encouraging the cell-to-cell propagation of tangle-susceptible tau protein in the brain. These results denote that AQP4 could be a powerful target for therapy in the context of tauopathic dementias.
Before delving further, here are other ways the brain can housekeep itself.

All of these events occur at a macro level, meaning outside the cell, and inside our cells, we have many other systems, I will briefly present you with a recent article and an amazing recent paper on the micro level, inside the cell.
Study finds new pathway for clearing misfolded proteins
In a new study published April 20 in Nature Cell Biology, researchers at Stanford University discovered a previously unknown cellular pathway for clearing misfolded proteins from the nucleus, the compartment where the cell stores, transcribes, and replicates its DNA. Keeping junk away from those processes is critical to normal cellular function. The new pathway could be a target for age-related disease therapies.
To find the new pathway, researchers in the lab of Judith Frydman, the Donald Kennedy Chair in the School of Humanities and Sciences, integrated several genetic, imaging, and biochemical approaches to understand how yeast cells dealt with misfolded proteins. For the experiments, the team restricted misfolded proteins to either the nucleus or the cytoplasm – the area inside the cell but outside the nucleus. The team visually followed the fate of the misfolded proteins through live-cell imaging and super-resolution microscopy.
“The first exciting thing was that we actually found that there’s communication between the nucleus and the cytoplasm,” said Emily Sontag, the co-lead author of the paper and a former postdoctoral student in the Frydman Lab. “So they’re telling each other, ‘We both have a lot of misfolded proteins; let’s coordinate to send them here to this garbage dump so that they can be removed.’”
The team identified the “garbage dump” site as the intersection of the nucleus and the vacuole – an organelle full of enzymes for degrading proteins – and showed that misfolded proteins in this “garbage dump” site are moved into the inside of the vacuole for degradation. They also showed that the pathway depends on a class of proteins used to create small vesicles for transporting molecules around cells.
“Tying that particular family of proteins and this aspect of vesicle traffic biology to protein clearance gives us a new way to look at Alzheimer’s, Parkinson’s, Huntington’s – all these neurodegenerative diseases,” said Sontag.
Alternative systems for misfolded protein clearance: life beyond the proteasome

Inside our cells, besides quite a few other intricate mechanisms, we have the Protein Quality Control (PQC) system and the Ubiquitin System. The Protein Quality Control (PQC) system is a highly sophisticated responsible for monitoring, maintaining, and ensuring the proper folding, function, and degradation of proteins within the cell.
In instances where proteins are irreversibly misfolded or damaged, the PQC system employs a process known as proteolysis for their removal. The proteasome, a large protease complex, is a central player in this process. Ubiquitin, a small protein, is attached to misfolded or damaged proteins, marking them for recognition and subsequent degradation by the proteasome.
The ubiquitin system is a fundamental regulatory mechanism in cells that governs protein degradation, among other cellular processes. Ubiquitin, a small protein consisting of 76 amino acids, acts as a molecular tag that is covalently attached to target proteins, marking them for degradation or influencing their cellular localization and activity. It is involved in various cellular processes, including cell cycle progression, DNA repair, signal transduction, and the removal of misfolded or damaged proteins through the aforementioned PQC system.
Your body is an amazing resilient marvel of life, and hopefully, with this, you are now aware of how your body is constantly dealing with misfolded proteins, how multiple steps play a role, how the glymphatic system works, and a brief explanation of how inflammation affects your brain’s housekeeping.
I will inevitably write part 2 soon since this one is already long and a little bit complicated, I didn’t cover antioxidants (NRF2 especially), sleep deprivation, the Kynurenine Pathway, or the role Herpes viruses play in this.
I am very grateful for your support !




I abide by my "no bad vibes in late December" rule even if it hurts me financially, which is ironic since in the last 10 days over half a dozen papers were published providing evidence to many of my observations, some related to the topic at hand. They are inevitably "bad vibes".
I may publish unrelated articles to Covid or health, thoughts on other subjects before the year's end, and a e-mail on Christmas, but besides that, patience is appreciated, I refuse to publish negative, doom and gloom stuff for the remainder of this year.
January 2024, we hit the ground running 🫡
Also take a look at this review paper regarding the influence of the upregulated MAO enzyme activity that comes with increasing age and is thought to be at the root of PD and AD: https://sci-hub.ru/10.1016/j.arr.2021.101256. I don't know about metformin or berberine, but quercetin -- available in foods and in supplement form -- significantly inhibits elevated MAO activity (not to mention that of CD38).