As I wrote a few days ago, this one will be short, or as we used to say “slow is smooth, smooth is fast”. For further context, any reader interested would benefit from reading the articles below.
In the past few months, I have written and researched, to a good extent the interplay and potential contribution of SARS-CoV-2 (and its vaccines, obviously), latent viruses, and both Long Covid and the damage induced by severe infection (which the vaccine mimics via dozens of pathways).
A few timely papers further brought to attention the role of Covid infections and vaccination also play in viral reactivation. Sadly I couldn’t find any of the normal ways to circumvent the paywall, but the abstract is enough in this particular case.
Here we have multiple interesting points. First, there has been an idea that Covid infection and vaccination caused unique skin lesions, and here they present results that diminish that concept. Secondly, vaccinated people had 2 times the chances of developing herpetic lesions, meaning viral reactivation of Herpesviruses that cause skin. Also, this little fact may bother some… “doctors”.
Increased Myocardial Infarction Risk Following Herpes Zoster Infection
Herpes zoster infection was associated with an increased risk of MI within the first 30 days postinfection. History of prior MI, male sex, age ≥50 years, history of heart failure, peripheral vascular disease, human immunodeficiency virus, prior cerebrovascular accident, and renal disease increased odds of MI 30 days postinfection with herpes zoster.
You can read why I am interested in Herpesviruses and the complex role they play here because they are underappreciated but significant contributors to both acute (aggressive, fast) and long-term damage to the body. The perfect virological example of “slowly, but surely” if you ask me. For the following paper:
Preliminary Evidence of the Differential Expression of Human Endogenous Retroviruses in Kawasaki Disease and SARS-CoV-2-Associated Multisystem Inflammatory Syndrome in Children
The title speaks for itself and is a timely finding, in line with recent propositions and findings (both from researchers and myself). Given the complexity of both diseases, MIS-C and Kawasaki’s, it is a step in a promising direction in finding the potential role of HERVs in both hyperinflammatory states.
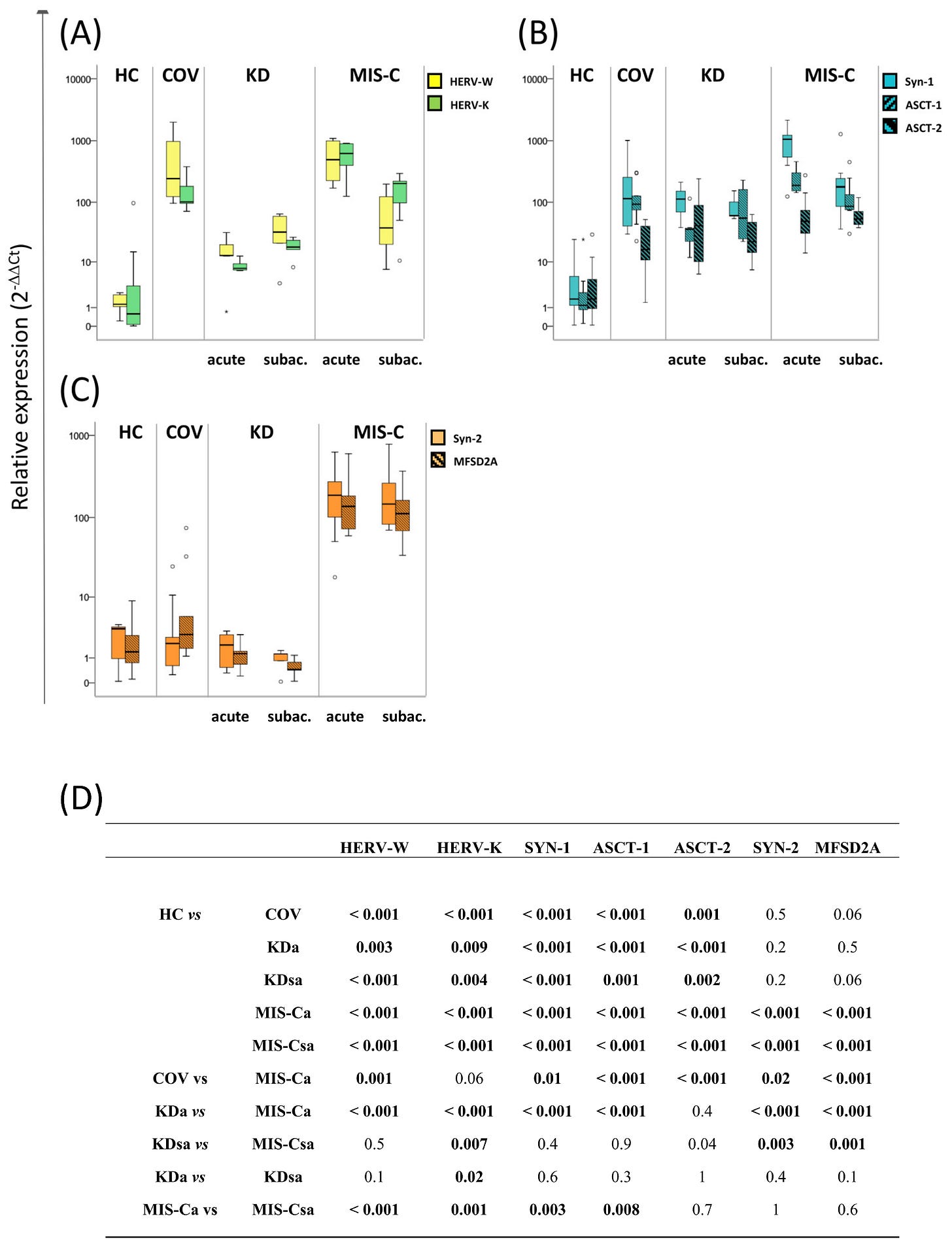
In a small group of children, first, they decided to measure the levels of specific genes related to HERVs, since this has been their central interest for a while (Thank God for that). Here they found higher levels of HERV-W and K (“bad HERVs”, because remember, they play multiple roles and some HERVs can be protective) Syn-1, and ASCT-1 and 2 were found in blood samples from KD, MIS-C, and COV patients, while higher levels of Syn-2 and MFSD2A were found only in MIS-C patients, regardless of the disease phase. Different states of the disease (subacute x acute phase) had different levels of expression of each of these markers.
Next, they measured the correlation between inflammatory and regulatory cytokines, and how how they might differ. When it came to Toll-Like Receptors, only Covid infection and both states of MIS had significant levels.
In Covid infected children, higher levels of IL-6, MCP-1 (both inflammatory), IL-10 (anti-inflammatory), TLR-3, and 9 were found, while TNF-Alpha (it can be both, inflammatory or anti) was found to be higher in Acute MIS. Comparing acute cases of Kawasaki and MIS, MIS had TNF-Alpha at higher levels, while Kawasaki had IL-10. IL-10 and MCP-1 were found higher in subacute MIS compared to Kawasaki.
In regards to disease progression, in Kawasaki higher levels of IL-10, TNF-Alpha, and MCP-1 were found in the acute phase compared to subacute. In MIS, higher TNF-Alpha, TLR-3, 4, 7, and 9 were found in the acute phase compared to the subacute, while IL-6 and IL-10 levels were higher in the subacute phase.
The findings here tell us a lot. First, there is a general deregulation of the transcriptional activity (being produced by your cells) of HERVs, its byproducts, and its receptors as well its inflammatory mediators, meaning inflammatory proteins that can contribute to the expression of these forgotten virus pieces.
Both HERV W and K can contribute to disease and inflammatory progression and are found in different tissues in severe Covid patients. Early higher levels of HERVs in Covid infection are a very good predictor of disease severity. It is interesting that the authors did not find an abundance of TLR in Kawasaki, but they found higher levels in both Covid infection and MIS, expected given how many parts of the virus and the subsequent damage it does to cells can engage the TLRs and start inflammatory responses.
What does the information above tell us, besides similarities and differences between both hyper-inflammatory diseases is how they progress, in the subacute phase of both diseases, despite different proteins being expressed, they are both in an “anti-inflammatory” state, and in the acute state both are in an obviously highly inflammatory state.
There is a dynamic shift in immune response in both diseases, and the body is attempting very hard to limit the inflammatory response. In that regard, the higher the levels of IL-10 in Acute MIS-C patients, the lower the levels of HERV-W.
HERV-W can create inflammatory feedback loops piggybacking on initial inflammatory responses, thus creating an endless cycle of both short-term aggressive inflammation and long-term low-grade one.
It would be incredibly beneficial to further understand both diseases and Covid in general, if they further tested the samples of all children for herpesviruses, fungal or bacterial infections, or just for different superantigens, given how many of the markers measures here are also responsible for “cytokine storms” the immunological byproducts of superantigen exposure.
While both are very rare conditions, and MIS-C is a very new one, it would be interesting if further research was done in relation to Kawasaki and the brain, focusing on the possible role of the disease in the long-term development of neurodegeneration. HERVs play a central role in protein misfolding, and they play a significant role in MIS and KD… this is my cue to finish and publish the HERVs-Protein misfolding article.









At the time MIS-C was discussed as Kawasaki like syndrome of COVID in children I became aware of some link to reappearing “inflammation” around the fully scarred BCG vaccine injection site ( Bacillus Calmette-Guerin (BCG) is the live attenuated vaccine form of Mycobacterium bovis used to prevent tuberculosis and other mycobacterial infections.). Would be interesting to see a link between BCG and HERVs. Did not search.
On the practical side, I concluded that sufficient Vitamin D would prevent.
I don’t have the support at hand, but both links are easily found when searched specifically in the literature.
Excellent work. Some of the clinical manifestations of MIS-C mimic Kawasaki disease (KD). That aside, S-protein is the master of mimicry, anti-S IgA is the "bus driver" your looking for, just a "gut" instinct Professor.