Just to be abundantly clear, I am not the first person able to go down this road, there were a few researchers ostracized by everyone talking about the role of KP and NAD in 2020. These are the true visionaries.
Unlike the Paradoxical Acquired Immune Dysfunction hypothesis, which we were fairly confident about since the inception and start of the research, this is more like an exploration, even though given the extension and amount of evidence presented, it will feel like a hypothesis. I personally believe this is one of the main drivers of disease and sequelae among many of those who died or are afflicted with Long Covid.
The paragraph above was written weeks ago, and I will maintain it, but now it is most likely a theory than a hypothesis. Just keeping a track record of some sort. Firstly, I will explain what the Kynurenine Pathway is, after I will cover its role on SARS-CoV-2, and build from there.
The kynurenine pathway is a metabolic pathway leading to the production of nicotinamide adenine dinucleotide (NAD+).[1] Metabolites involved in the kynurenine pathway include tryptophan, kynurenine, kynurenic acid, xanthurenic acid, quinolinic acid, and 3-hydroxykynurenine.[1][2] The kynurenine pathway is responsible for total catabolization of tryptophan about 95%.[3]
The Kynurenine pathway is one of the most important pathways in regards to both health and disease, since it is intrinsically linked to the metabolism of one of the most essential amino acids to life, Tryptophan (you can’t function without tryptophan). The kynurenine pathway, the enzymes you need and its metabolites (byproducts of your body processing it) all play a different role in your overall health. From your blood vessels to the immune system, and especially and of great interest to medicine lately, cognitive/brain function.

That is what a “metabolic” pathway looks like. To understanding why NAD+ is part of this is so important, this will bring light to it.
And of course, I have been hinting at the KP for a long time and how it ties into this entire thing.
A lot of other posts play a heavy part in this, but to avoid overcomplicating this, I will try to make it super simple. When your body runs out of NAD+ (needs it to make “cell energy”) it will activate alternative pathways to get the NAD, the body always does this with many other necessary building blocks of our bodies. The KP is this alternative pathway, which will deplete Tryptophan, in turn, the inflammation and more production of KP will kinda set some people into a loop.
And with that out of the way, we look into if there is any sign of the KP being really that active in regards to SARS-CoV-2
Kynurenine pathway in Coronavirus disease (COVID‐19): Potential role in prognosis
By measuring specific metabolites on the Kynurenine pathway, these researchs found that severe patients had a higher ratio of picolinic acid can become neurotoxic in larger quantities, IL-6 is an inflammatory protein, and if you read they PAID hypothesis you should be familiar with the concept that ratio among cells or anything inside you is important, a skewed ratio towards Kynurenine from Tryptophan causes a whole host of problems. But we must go deeper.
The tryptophan catabolite or kynurenine pathway in COVID-19 and critical COVID-19: a systematic review and meta-analysis
Coronavirus disease 2019 (COVID-19) is accompanied by activated immuneinflammatory pathways and oxidative stress, which both may induce indoleamine-2,3- dioxygenase (IDO), a key enzyme of the tryptophan (TRP) catabolite (TRYCAT) pathway. The aim of the current study was to systematically review and meta-analyze the TRYCAT pathway status including levels of TRP and kynurenine (KYN) and IDO activity, as assessed using the KYN/TRP ratio.
In our metaanalysis we included 14 articles which examine TRP and TRYCATs in COVID-19 patients versus non-COVID-19 controls, and severe/critical versus mild/moderate COVID-19. Overall, the analysis was performed on 1269 individuals, namely 794 COVID-19 patients and 475 controls. The results show a significant (p <0.0001) increase in the KYN/TRP ratio
The TRYCAT pathway is probably implicated in the pathophysiology and progression of COVID-19 and may signal a worse outcome of the disease
These results indicate that IDO activity and the TRYCAT pathway are upregulated in COVID-19 and that it predicts critical disease and non-survival. The most probable cause of IDO enzyme activation in COVID-19 is the increased level of pro-inflammatory cytokines including IFN-γ, IL-1β and IL-6 (Akbari, Tabrizi et al. 2020, Mulchandani, Lyngdoh et al. 2021) and activated oxidative stress pathways
Further analyses showed that the changes in the KYN/TRP ratio are attributable to significant increases in KYN and decreases in TRP in COVID-19 again with large effect sizes. These results extend the findings of previous studies which showed associations between severity of COVID-19 and increases in the KYN/TRP ratio and KYN and decreases in TRP
So a meta-analysis (you basically go through a large amount of literature, and see if and where trends come up, merging the findings, in my opinion, is the best approach when it comes to research, especially if you do interdisciplinarily) found something similar as the paper above. A substantial skewed ratio towards Kynurenine, decreases Tryptophan, the imbalance sets of multiple inflammatory responses, and starts producing less NAD (cell energy) and more toxic metabolites.
Now to the paper that actually started making everything click for me after MONTHS of being lost into this damn pathway.
Post-acute COVID-19 cognitive impairment and decline uniquely associate with kynurenine pathway activation: a longitudinal observational study
Cognitive impairment and function post-acute mild to moderate COVID-19 are poorly understood. We report findings of 128 prospectively studied SARS-CoV-2 positive patients. Cognition and olfaction were assessed at 2-, 4- and 12-months post-diagnosis. Lung function, physical and mental health were assessed at 2-month post diagnosis. Blood cytokines, neurobiomarkers, and kynurenine pathway (KP) metabolites were measured at 2-, 4-, 8- and 12- months. Mild to moderate cognitive impairment (demographically corrected) was present in 16%, 23%, and 26%, at 2-, 4- and 12-months post diagnosis, respectively. Overall cognitive performance mildly, but significantly (p<.001) declined. Cognitive impairment was more common in those with anosmia (p=.05), but only at 2 months. KP metabolites quinolinic acid, 3-hydroxyanthranilic acid, and kynurenine were significantly (p<.001) associated with cognitive decline. The KP as a unique biomarker offers a potential therapeutic target for COVID-19-related cognitive impairment.
Note from me - Olfaction is literally the act of smelling, or capacity to
The change and higher levels of certain metabolites of the KP were found even after 12 months in persons with Long Covid (they now refer to it as PASC), and levels are correlated with the decline, which isn’t a major decline, but perceptible and it will affect daily life (aka the now infamous brain fog).
Next, we elected to test the components of the plasma kynurenine pathway (KP) which is an IFN stimulated myeloid cell mediated tryptophan degradation pathway important in immune tolerance, neurotoxicity, and vascular injury.
First, you should write that myeloid down, then maybe Google it, but definitely write it down. It has major importance later on… if you can connect the dots, you already know the answer (dots are somewhere in my Twitter feed). Also, a reminder that this pathway.
Another important aspect of the KP is the fact that it relies on IDO, an enzyme needed to metabolize tryptophan into kynurenine, and it is upregulated by some physiological aspects, among one of the major ones, Interferon Gamma. That Interferon the vaccine pushes to eleven, and infection too sometimes… see some sort of problem ? Nah, must be my mind.
Urine metabolomics links dysregulation of the tryptophan-kynurenine pathway to inflammation and severity of COVID-19
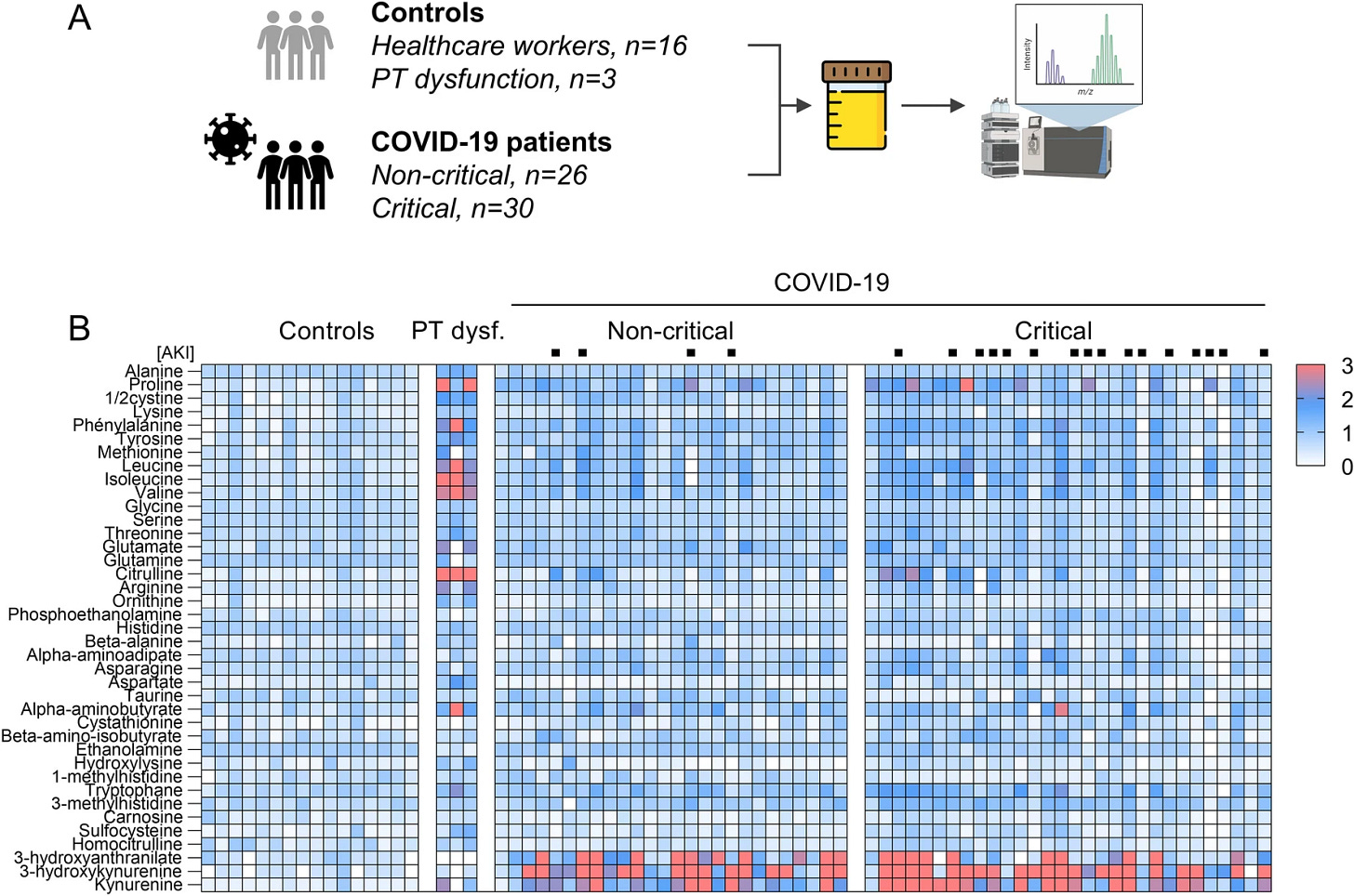
Metabolomic profiling revealed a major urinary increase of tryptophan metabolites kynurenine (P < 0.001), 3-hydroxykynurenine (P < 0.001) and 3-hydroxyanthranilate (P < 0.001) in SARS-CoV-2 infected patients. Urine levels of kynurenines were associated with disease severity and systemic inflammation (kynurenine, r 0.43, P = 0.001; 3-hydroxykynurenine, r 0.44, P < 0.001). Increased urinary levels of neutral amino acids and imino acid proline were also common in COVID-19, suggesting specific transport defects. Urine metabolomics identified major alterations in the tryptophan-kynurenine pathway, consistent with changes in host metabolism during SARS-CoV-2 infection. The association between increased urinary levels of kynurenines, inflammation and COVID-19 severity supports further evaluation of these easily available biomarkers.
(Someone on Twitter asked me about urinary tests on KP, so here, there is a published peer-reviewed paper stating that following their methods you get results because most other papers are relegated to blood/serum tests).
This is a very important paper, by the simple fact that they also measured non-critical patients.
As you can clearly see, there is a substantial presence of KP metabolites both in critical patients and non-critical alike, while health control has none (shades of blue to white=low to 0, the redder the higher).
Urine levels of kynurenines, systemic inflammation and severity of COVID-19
Among patients with COVID-19, the level of these urinary metabolites was also associated with disease severity, and patients with critical COVID-19 had higher levels of urinary tryptophan metabolites than those with non-critical disease . Systemic inflammation assessed by CRP levels at the time of sampling was tightly correlated with urinary concentration of kynurenine (Spearman, r 0.43, P = 0.001) and 3-hydroxykynurenine (r 0.44, P < 0.001), as well as with the kynurenine to tryptophan ratio
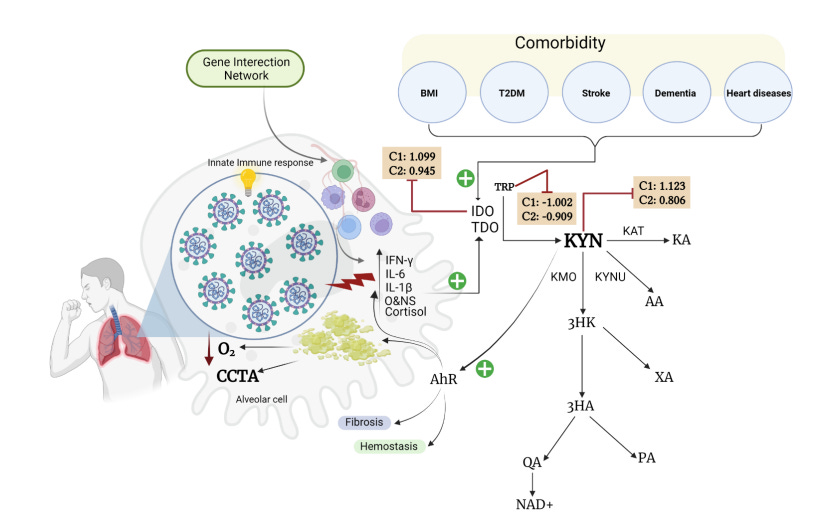
And here we have a good breakdown of how the KP works, and what it can do to your body, especially when IDO is activated, IDO can act as a strong immunosuppresor. This could explain in parts why some people can’t get rid of viral fragments inside them, and the persistent antigenic stimulation. It is a literally dysfunctional bioenergetic loop.
IDO is activated, immunosupress you, not enough immune cells to clean the viral debris, depletes your NAD, repeats, stays in a permanent state of immune dysfunction and “half voltage”. IDO also raises your oxidative stress level, further depleting people of antioxidants, especially Glutathione.
Per the paper above, and proved by others we covered here, there is a long-term change in the metabolism of Tryptophan in many people that recover from SARS-CoV-2, and this created a skew in the KYN:TRP ratio. This is merely to drive my point.
Here are some of the following roles of KP in diseases.

This piece is long and complex enough as it is, I will cover the many, many pathologies that are fueled by KP, this was mostly to introduce you to this pathway, and its importance, which will be crystal clear in the next parts, and the complete pathway.
And once again, one of the most important aspects of this is the mitochondria. Of course, a high carbohydrate diet will skew you heavily towards the toxic metabolites we are discussing here. Guess which type of diet inhibits and fixes these issues ?
I will leave it to your imagination and if you paid attention to anything I wrote so far…
Have a good weekend everyone !
A very big thank you to all supporters here and those who use KoFi =) !







This ties very very VERY closely to the following posts.
https://hiddencomplexity.substack.com/p/omicron-evasion-sars-cov2-and-the
https://hiddencomplexity.substack.com/p/sars-cov-2-the-brain-and-the-sugar
https://hiddencomplexity.substack.com/p/sars-cov-2-the-brain-and-amyloid
Due to the GP120 & GAG inserts I thought I would do a cross reference. Bingo!
I already considered NAD but not your kynurenine pathway, I will now need to add this to my review.
Note the doom loop you also referred to and the need to break the cycle with therapeutics.
Clinical Relevance of Kynurenine Pathway in HIV/AIDS: An Immune Checkpoint at the Crossroads of Metabolism and Inflammation
Jean-Pierre Routy et al. AIDS Rev. 2015 Apr-Jun.
Abstract
Tryptophan degradation along the kynurenine pathway is associated with a wide variety of pathophysiological processes, of which tumor tolerance and immune dysfunction in several chronic viral infections including HIV are well known. The kynurenine pathway is at the crossroads of metabolism and immunity and plays an important role in inflammation while also playing an opposing role in the control of acute and chronic infections. In this review we have summarized findings from recent studies reporting modulation of tryptophan degrading the kynurenine pathway in the context of HIV infection. This immuno-metabolic pathway is modulated by three distinct inducible enzymes: indoleamine 2,3-dioxygenase 1 and 2 and tryptophan 2,3-dioxygenase. Increased expression of these enzymes by antigen-presenting cells leads to local or systemic tryptophan depletion, resulting in a mechanism of defense against certain microorganisms. Conversely, it can also lead to immunosuppression by antigen-specific T-cell exhaustion and recruitment of T regulatory cells. Recently, among these enzymes, indoleamine 2,3-dioxygenase 1 has been recognized to be an immune response checkpoint that plays an important role in HIV immune dysfunction, even in the context of antiretroviral therapy. In addition to the activation of the kynurenine pathway by HIV proteins Tat and Nef, the tryptophan-degrading bacteria present in the intestinal flora have been associated with dysfunction of gut mucosal CD4 Th17/Th22 cells, leading to microbial translocation and creating a systemic kynurenine pathway activation cycle. This self-sustaining feedback loop has deleterious effects on disease progression and on neurocognitive impairment in HIV-infected patients. Therapy designed to break the vicious cycle of induced tryptophan degradation is warranted to revert immune exhaustion in HIV-infected persons.
https://pubmed.ncbi.nlm.nih.gov/26035167/#:~:text=The%20kynurenine%20pathway%20is%20at,of%20acute%20and%20chronic%20infections.
https://doorlesscarp953.substack.com/p/pathophysiology-of-spike-protein