Glycaemic control is associated SARS-CoV-2 breakthrough infections in vaccinated with type 2 diabetes
And the diabetes connection
Anyone who reads my posts about this virus, or health in general, is aware of my continuous mentioning of excessive carbohydrate consumption, and for quite some time many argued the impact of glycemic control on the immune response of the vaccine. It has been known for years that poor glycemic control (pre, and diabetes itself, insulin resistance, metabolic dysfunction) leads to poor immune response, among a long list of other physiological effects.
Glycaemic control is associated with SARS-CoV-2 breakthrough infections in vaccinated patients with type 2 diabetes
Patients with type 2 diabetes (T2D) are characterized by blunted immune responses, which are affected by glycaemic control. Whether glycaemic control influences the response to COVID-19 vaccines and the incidence of SARS-CoV-2 breakthrough infections is unknown. Here we show that poor glycaemic control, assessed as mean HbA1c in the post-vaccination period, is associated with lower immune responses and an increased incidence of SARS-CoV-2 breakthrough infections in T2D patients vaccinated with mRNA-BNT162b2.
Considering the 494 subjects completing the study, patients with good glycaemic control (HbA1c one-year mean < 7%) show a higher virus-neutralizing antibody capacity and a better CD4 + T/cytokine response, compared with those with poor control (HbA1c one-year mean ≥ 7%). The one-year mean of HbA1c is linearly associated with the incidence of breakthrough infections.
Glycated hemoglobin A1c is one of the best ways to measure sugar in your blood. Glycated means “linked to sugar”, usually proteins or lipids. With that out of the way, the “normal” levels vary in some countries but the maximum normal range is 5.7%, passed this you are considered diabetic, and clearly have insulin resistance. They measured such marker for a year, and the impact it has on antibody levels, a T cell response.
Beyond the effect of time on waning antibody titres and the emergency of viral variants escaping pre-existing immunity, also patient-intrinsic characteristics might influence immune responses to COVID-19 vaccines and thus the efficacy of vaccination
Authors recognize the other variables at play in the immune response.
Level of immune-related parameters according to glycaemic control
All participants were evaluated to assess their neutralization antibody responses and T-cell responses. T2D patients with HbA1c ≥ 7% showed a significantly reduced virus-neutralizing antibody capacity compared with T2D patients with GC, as assessed by the one-year mean of the percentage of neutralization
Moreover, in response to stimulation of peripheral blood cells with S-specific peptide pools, we observed a higher CD4+ T/ cytokine response involving type 1 helper T cells in patients with GC compared with PC, as demonstrated by a higher number (one-year mean) of CD4+ T cells expressing interferon (IFN)-γ (Fig. 2B), interleukin (IL)-2 (Fig. 2C), and tumour necrosis factor-(TNF) α (Fig. 2D) (one-year mean for all).
Pretty straightforward so far, right? Too much sugar floating around inside your blood, hinders your cell capacity to respond to other things, there are many mechanisms for why that happens, but to simplify to the layperson, the sugar molecules coat everything and make it hard for cells to do their thing.
Here they found that important markers were significantly reduced over a period of 1 year, in patients without proper glycemic control.
The intrinsic impossibility of vaccines to produce a 100% coverage against infections, the effect of time on waning antibody titres, and the emergence of viral variants escaping vaccine-induced immunity are likely the major determinants of vaccination failures4,5. However, also patient characteristics might influence the incidence of breakthrough infection, as suggested for patients with different comorbidities, including T2D6,7,8. Data presented here suggest that poor glycaemic control during the year after vaccination worsens the immunological response to the BNT162b2 vaccine and might favour SARS-CoV-2 breakthrough infections within T2D patients.
Now let us do, what we do around here.
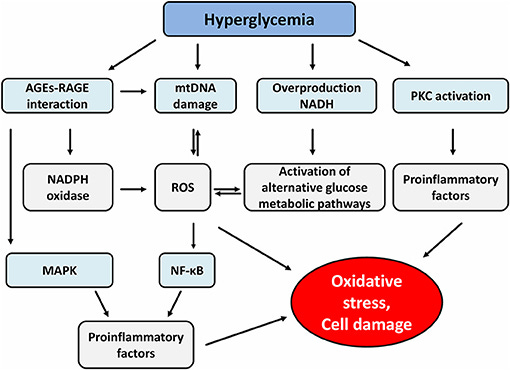
The Effect of Short-Term Hyperglycemia on the Innate Immune System
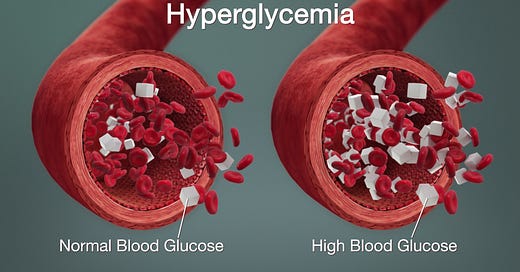
Under a hyperglycemic state (too much sugar floating around without use), it enacts precisely every advantageous state to foreign pathogens, and opportunistic infections to set in, and grow. Each and everyone one of these has an impact not only on your immune response but also on developing severe disease, long-term inflammation, etc.
Shor-term hyperglycemia doesn’t mean you became a diabetic, means you have been eating too much carbohydrates, not exercising much, and have lots of sugar floating around.
I could spend weeks writing 16 hours a day solely on this subject. Below a decent article about hyperglycemia and “leaky gut” and dysbiosis.
How Hyperglycemia Drives Gut Barrier Dysfunction and Dysbiosis
There is a massive discussion between scientists and clinicians if SARS-CoV-2 can cause new onset diabetes or not, and what are the mechanisms behind it. I will leave just a few papers here, to make my point later.
Acute and long-term disruption of glycometabolic control after SARS-CoV-2 infection
Glycaemic abnormalities can be detected for at least 2 months in patients who recovered from COVID-19. Our data demonstrate that COVID-19 is associated with aberrant glycometabolic control, which can persist even after recovery, suggesting that further investigation of metabolic abnormalities in the context of long COVID is warranted.
What the very least the viral infection impacts your glycemic metabolism via different mechanisms.
Risk for Newly Diagnosed Diabetes >30 Days After SARS-CoV-2 Infection Among Persons Aged <18 Years — United States, March 1, 2020–June 28, 2021
Persons aged <18 years with COVID-19 were more likely to receive a new diabetes diagnosis >30 days after infection than were those without COVID-19 and those with prepandemic acute respiratory infections. Non–SARS-CoV-2 respiratory infection was not associated with an increased risk for diabetes.
Newly developed type 1 diabetes after coronavirus disease 2019 vaccination: A case report
Exacerbation of hyperglycemia in patients with type 2 diabetes after vaccination for COVID19: Report of three cases
Both the viral infection, and the vaccines can induce poor glycemic control, and aid the dysfunction into becoming diabetes, my point in sharing these papers was meant to show you that, yes hyperglycemia and poor glycemic control impact the immune system, and your whole body, it is not solely because of diet, or other variables. The vaccination affects your hepatic (liver) functions, the viral infection also can impact that, you get a breakthrough infection that adds fuel to the fire.
For months I used social media to track down the thousands, upon thousands of tweets of people developing poor glycemic control after the vaccination, and after breakthrough infections.
For most people, Intermittent Fasting, and fasting, in general, are extremely helpful to revert these scenarios. For most diabetics, a low carbohydrate diet will put your “diabetes in remission”, it will fix most people's metabolic dysfunction. This post will make sense if you read others, especially Reverse AIDS, but a future one about Omicron BA. 4, and BA. 5. Read the Part III post to understand why a low carbohydrate diet is so helpful (fasting is the same too, it is just flooding you with ketones).
You can buy me a coffee whenever you feel like it.
Deep appreciation for all the supporters!








Thanks for highlighting diet and nutrition! I think that is the key to beating c19 along with a few supplements.
I am convinced that if people would just NOT eat processed food their health be multiplied... Stop seed oils, sugar and anything artificial, and health will be restored!
I'm pushing 75, low carb/keto/carnivore for 12 years. No meds and no chronic issues. Thanks again.
I was wondering why diabetics had more severe outcomes from the covid illness.
I love that gif! 💞💫
I intermittently fast fairly regularly, although I'm not pre-diabetic. I actually eat whole fruits and kale as a blended drink throughout the day for an easy source of energy. I recently had my blood sugars tested and they were low. I was on a keto diet for a while after being ill with who knows what, kind of chronic fatigue-ish (heavy metals, adrenal fatigue, Wi-Fi sensitivity, some food sensitivities). It seemed to help for a half a year, and then I began to get tired after every meal, and felt like the energy to digest the meal was more than what the meal provided. 10 years ago I shifted over to fresh fruits and vegetables with meats, and I had already cut out most all processed foods and unhealthy oils, and I've never felt healthier in my whole adult life. 👍🏼